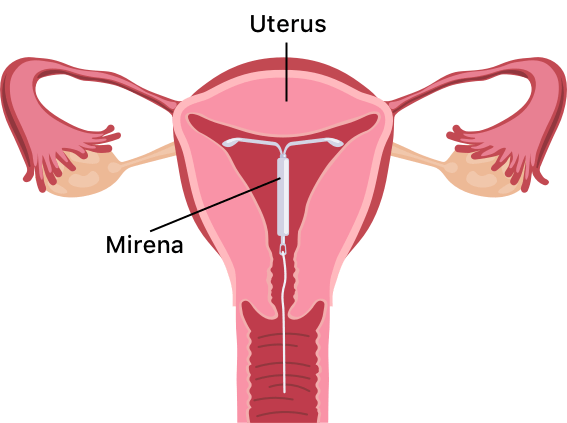
The Displacement of IUD: Causes, Effects, and Solutions
– Displacement of IUD
– Shifting out of place
– Partially or fully dislodged
– Risk factors for displacement
– Signs of displaced IUD
– Not able to feel IUD string
– String feeling shorter or longer
– Feeling IUD during sex
– IUD coming out of cervix
– Abdominal cramping
– Pain, discomfort
– Unusual vaginal discharge
– Heavier or atypical vaginal bleeding
– Fever or chills
– IUD no longer providing pregnancy protection
– Different form of birth control may be needed
– Emergency contraception
– Contact a doctor
– Pros of IUDs
– High effectiveness in preventing pregnancy
– No need to remember to take medication
– Easy reversibility
– Improvement of heavy periods and cramping
– Effectiveness as emergency contraception
– Cons of IUDs
– Painful insertion
– Changes in bleeding patterns
– Perforation leading to bleeding or infection
– Unintended pregnancy due to displacement
– Increased risk of ectopic pregnancy or septic abortion
– Consult with a doctor
– Effects on hormones
– Potential side effects or risks
– Protection against sexually transmitted infections
– Interactions with other health conditions, medications, or supplements
– IUDs do not protect against STIs
– Additional protection such as condoms needed
– Potential harm caused by out-of-place IUD
– Possibility of IUD falling out (expulsion)
– Feelings associated with IUD displacement
– Rate of expulsion
– Physical symptoms of IUD displacement
– Factors that increase the likelihood of displacement
– Checking if IUD has moved
– Washing hands, squatting or sitting, inserting a finger
– Feeling for string ends without tugging or pulling
– Steps taken by doctors to determine if IUD has moved
– Contacting a doctor or healthcare provider
– Examination and tests
– Emergency contraception and backup method
– Decision to remove or leave IUD
– Ultrasound to locate IUD
– X-ray if IUD cannot be found
– Laparoscopic procedure for removal and replacement
– Alternative birth control options
– Doctor may see IUD in cervix
– Pros and cons of using an IUD
– IUD effectiveness
– Long-lasting form of birth control
– Reversibility and possibility of pregnancy after removal
– Benefits of hormonal IUDs
– Benefits of copper IUDs
– Cost comparison to other methods
– Pain during insertion and removal
– Increased risk of ectopic pregnancy
– Effects of copper IUD on periods and cramps
– Risk of pelvic inflammatory disease
– Rare possibility of uterine perforation